Your smile feels like a memory after years of struggling with failing teeth and a shrinking jawline. You might think the window for a permanent fix closed long ago because your dentist mentioned your bone is too thin. But that isn’t true anymore. Modern restorative techniques mean that even if you’ve been told no before, can you get dental implants with severe bone loss in jaw is a question that now has a resounding yes for an answer. You can move from hiding your mouth to eating a steak with total confidence. Technology has finally caught up to your needs.
How does bone loss affect your ability to get dental implants?
Bone loss is a silent thief. When you lose a tooth, the jawbone no longer receives the stimulation it needs from chewing forces. It begins to resorb, which is a fancy way of saying your body dissolves the bone and uses the minerals elsewhere. This process happens quickly, with significant volume vanishing within the first year of tooth loss.
Traditional implants need stable ground. They work like a screw in a wall. If the drywall is crumbling, the screw won’t hold the weight of the picture. For years, surgeons required a specific height and width of bone to ensure the titanium post would fuse properly. This process is called osseointegration. Without it, the implant fails.
But your jaw isn’t the only support structure in your face. Surgeons now look at the entire craniofacial architecture. They check the density of your remaining bone. They measure the gap. They find a way.
Can you get dental implants with severe bone loss in jaw using bone grafting?
Grafting is the classic solution for rebuilding what time took away. It involves taking bone material and placing it where your jaw has thinned out. Your body uses this material as a scaffold. It grows new, living bone through the graft. This creates a solid foundation.
You have several options for graft material. Some people choose their own bone, often taken from the chin or hip. Others prefer lab-processed materials or mineral-based substitutes that carry zero risk of second-site surgery. These materials are incredibly effective in 2026. They’re designed to be absorbed as your natural bone takes over.
Healing takes time. You shouldn’t rush the process. Usually, you’ll wait three to six months for the graft to solidify. Only then will the surgeon place the implant. It’s a journey. It’s an investment in a lifetime of chewing.
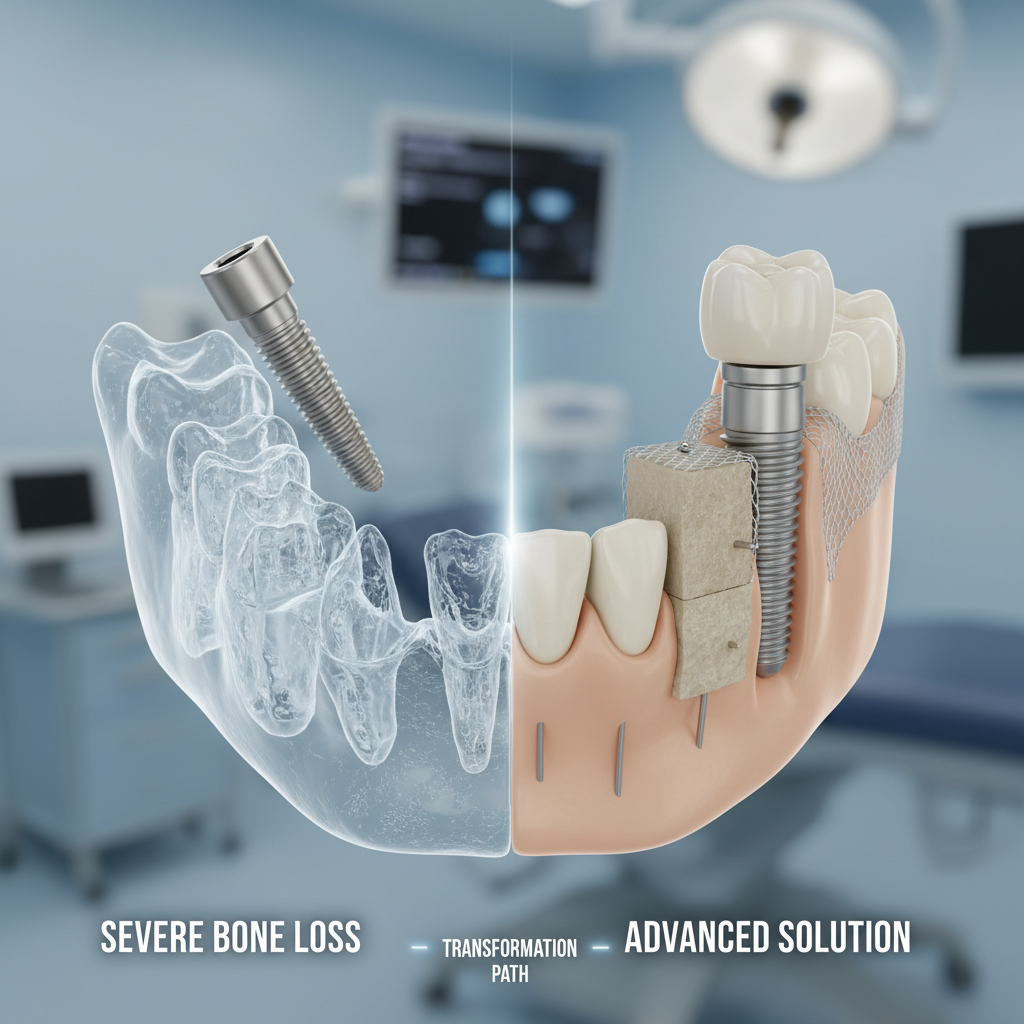
Are zygomatic implants the right choice for upper jaw bone loss?
If your upper jaw is paper-thin, you might bypass the jawbone entirely. Zygomatic implants are longer than standard ones. They don’t anchor in the maxilla. Instead, they reach up and anchor into the zygomatic bone, which most people know as the cheekbone.
The cheekbone is incredibly dense. It doesn’t resorb like the jawbone does. This makes it an ideal anchor for people who have been told they have zero chance of traditional implants. You don’t usually need bone grafting for this procedure. It saves months of waiting.
This is a specialized surgery. You need a surgeon with extensive experience in maxillofacial reconstruction. It’s often done under general anesthesia. You wake up with a temporary bridge already in place. The results are life-changing.
Is the All-on-4 technique effective for patients with low bone density?
Traditional methods often required six or eight implants per arch. That’s a lot of bone needed. The All-on-4 approach changed the math by using just four strategically placed posts. Two are placed straight in the front. Two are tilted at a 45-degree angle in the back.
This tilt is the secret. It allows the surgeon to use the thickest part of the bone near the front of the mouth. It avoids the need for sinus lifts in the upper jaw. It maximizes every millimeter of available structure. You get a full set of teeth on just four pillars.
Stability is immediate. Because the implants are connected by a rigid bridge, they support each other. You can often get your new teeth on the same day as the surgery. It’s efficient. It’s predictable.
What role does 3D imaging play in planning implants for thin jawbones?
We don’t guess in 2026. Every procedure starts with a CBCT scan. This creates a three-dimensional map of your skull. Your surgeon can see exactly where the nerves sit. They can measure the bone density to the fraction of a millimeter.
Virtual surgery happens before you ever sit in the chair. The doctor uses software to place the implants on the screen. They find the exact angle where the bone is strongest. They can even 3D print a surgical guide. This guide fits over your gums and shows the drill exactly where to go.
This precision reduces trauma. Less trauma means less swelling. It also means the surgeon can utilize tiny pockets of bone that would be impossible to find with a standard X-ray. Technology minimizes the risk. It maximizes the success rate.
Will a sinus lift help if there is not enough bone in the upper back jaw?
The upper back jaw is a tricky neighborhood. The sinus cavities sit right above your molars. When those teeth are gone, the bone stays thin, and the sinus expands downward. There isn’t enough room to put an implant without hitting the sinus membrane.
A sinus lift solves this. The surgeon delicately lifts the membrane upward. They tuck bone grafting material into the newly created space. Think of it like adding an extra layer of insulation in an attic. It creates the depth needed for a secure implant.
The success rates are very high. People often fear the recovery, but it’s manageable. You’ll avoid blowing your nose for a few weeks. You’ll take some decongestants. Soon, you’ll have enough bone to support those crucial back molars.
How do basal implants differ for people with extreme bone resorption?
Basal implants are different. Standard implants sit in the soft, spongy alveolar bone. Basal implants go deeper. They anchor in the basal bone, which is the hard, cortical part of your skeleton. This bone is resistant to infection and resorption.
This method is often called cortical implantology. It’s excellent for heavy smokers or people with controlled diabetes. The bone here is so strong that the implants can be loaded with teeth immediately. You don’t wait for months of grafting.
This technique is less common in some regions but gaining popularity. It requires a specific skill set. It provides a solution when the alveolar bone is completely gone. You finally have an alternative to loose dentures.
Why should you choose implants over dentures when bone is failing?
Dentures don’t stop bone loss. They actually speed it up. As the denture rubs against the gums, it puts pressure on the underlying ridge. This constant irritation causes the bone to melt away even faster. Your face begins to look collapsed.
Implants do the opposite. They act like natural tooth roots. By mimicking the pressure of real teeth, they signal the body to keep the bone healthy. Can you get dental implants with severe bone loss in jaw patients? Yes, and doing so often saves what bone you have left.
The psychological impact is huge. No more messy adhesives. No more worrying about your teeth falling out during a laugh. You regain your sense of taste because the roof of your mouth isn’t covered by plastic. It’s about quality of life.
What is the expected recovery time after dental implant surgery with grafting?
Patience is your best tool here. If you need a significant graft, the initial healing takes about ten days. This is when the stitches stay in. You’ll eat soft foods and keep the area clean. The real work happens underneath the surface for months.
The bone needs to mature. If you rush it, the implant might wobble. Once the bone is ready, the implant surgery itself is remarkably quick. Pain is usually less than what you feel after a tooth extraction. Most people return to work in two days.
Final restorations come last. After the implant fuses, your dentist crafts your custom teeth. These aren’t just functional. They’re pieces of art designed to match your face. The wait is worth the results.
Are there risks associated with performing implants in limited bone?
Every surgery has risks. The main concern with thin bone is nerve damage or sinus perforation. However, with the 3D planning we use today, these risks are minimal. Your surgeon sees the danger zones before they start.
Primary stability is the goal. If the implant doesn’t feel tight on day one, the surgeon might wait. They may add more graft and try again later. Resilience is key. A failed implant isn’t the end of the road.
Choosing the right specialist is your biggest safeguard. Don’t go to a generalist for complex bone loss cases. You need a periodontist or an oral surgeon. They have the training to handle complications. They know how to work with the bone you have.
How much do dental implants for severe bone loss typically cost?
Quality isn’t cheap. When you add bone grafting or zygomatic techniques, the price goes up. You’re paying for specialized materials and advanced surgical expertise. It’s a high-tech reconstruction of your face.
Check your insurance carefully. Many plans now cover the reconstructive part of the surgery even if they won’t pay for the teeth. Financing is also widely available. Most offices offer monthly payments that fit a budget.
Look at the long-term cost. Dentures need relining every few years. They need replacement every decade. Implants are designed to last the rest of your life. They’re the most cost-effective solution over twenty years.
Steps to reclaim your smile today
Stop waiting for the bone to grow back on its own. It won’t happened. Schedule a consultation with a specialist who uses 3D guided surgery. This is the only way to get a real map of your jaw. Knowledge is power.
Ask about all the options. Don’t settle for you aren’t a candidate until you’ve spoken to someone who performs zygomatic or All-on-4 procedures. Modern dentistry is about finding the yes. You’re one scan away from a new plan.
Prepare your body. If you smoke, try to quit or cut back. Boost your vitamin D and calcium levels. A healthy body builds better bone. You are the most important part of the healing team. Take that first step and book an assessment to see if can you get dental implants with severe bone loss in jaw surgery is the right path for you.
Frequently asked questions about dental implants and bone loss
Can I get implants if I have osteoporosis?
Yes. Osteoporosis affects the whole body, but the jaw bone is often still dense enough for implants. Your surgeon will coordinate with your physician. They will check if your medications, like bisphosphonates, affect the healing process. Most patients with osteoporosis successfully receive implants.
Does bone grafting involve a long hospital stay?
No. Most bone grafting for dental implants is an outpatient procedure. It’s done in the dental office with local anesthesia or IV sedation. You go home the same day. Recovery involves resting at home for a few days with ice packs and soft foods.
How do I know if I have severe bone loss?
You might notice your dentures feel loose. Your face may appear shorter between the nose and chin. However, the only certain way to know is through a CBCT scan. This imaging shows the bone height and width that a standard mirror cannot see.
Are zygomatic implants more painful than regular ones?
The surgery is more involved, so you’ll usually be sedated. This means you won’t feel anything during the procedure. Post-operative discomfort is manageable with prescribed or over-the-counter pain relief. Most patients report that the swelling is the most annoying part, not the pain.